The beauty of trauma care: What it means to be human
Scouring through chemical equations in textbooks, using laboratory instruments to probe the molecular signatures of cancer cells, and preparing for an exam that will encompass over ten subjects from organic chemistry to literary reasoning are all excellent descriptions of my daily life. I’m a fourth-year undergraduate at the University of Minnesota, and I want to become a physician-scientist. For students like myself who will be training for many years in highly developed fields, it is important to have a strong foundation in academic coursework and basic research experience before developing expertise in later stages. Yet I also think that during this early phase, it is equally critical that we learn how to maintain perspective as to why we’re doing all this in the first place – what motivates us to sacrifice weekends, lose sleep, and constantly push ourselves to learn more. As such, on Friday nights, I let go of all concerns about assignments and immerse myself in the setting I dream of someday helping people in — a setting that is over ten years of training away and yet pervades my every thought and action: I go to Hennepin County Medical Center’s Emergency Stabilization Room.
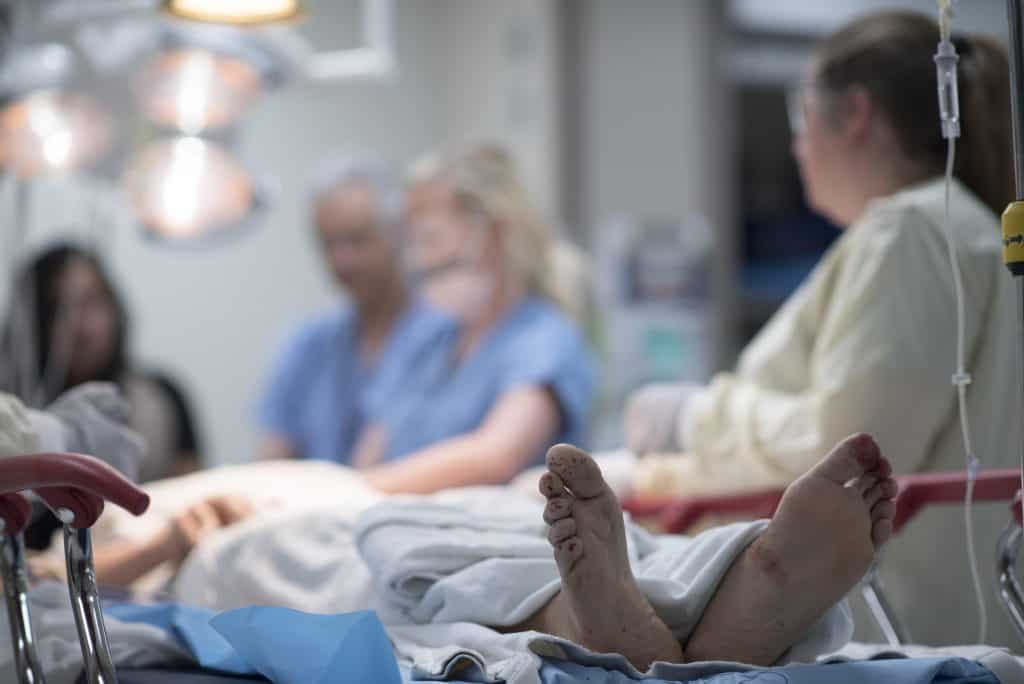
When someone experiences a dire medical emergency or traumatic injury and they are brought to HCMC, they go to what’s called the “stabilization room.” Most people don’t know that this room exists, but the patients who require it suddenly find they have gained an all-access pass as its guest of honor. Upon entering the stabilization room, located within the emergency department, one first notices partitions dividing the room into quadrants, each with its bed to accommodate a critical patient, and illuminated by piercing white light. It is not unlike how one might imagine the inside of an alien spaceship to appear. Adorned with an incredible density of state-of-the-art technology, this room is capable of handling every type of emergency procedure imaginable.
 As soon as a call comes into the HCMC emergency department that a patient who requires this level of care is inbound, an overhead page goes out through the department intercom: “Stab. Room personnel to the Stab. Room, trauma, ten minutes; Stab. Room personnel to the Stab. Room, trauma, ten minutes.” Doctors, nurses, and healthcare assistants make their way over to the stabilization room, key their card in, and begin preparing. The doctors and nurses don special isolation scrubs and prepare instruments and devices for the incoming patient, and depending on how much or little is known about the injury or illness that has occurred, healthcare assistants may alert other specialties that are on-call 24/7 in the hospital. Specialties called on include trauma surgery, neurosurgery, orthopedic surgery, radiology, the stroke team, the pediatric team, the burn team, and even a team that uses a bariatric chamber to treat carbon monoxide poisoning. In this way, what most often begins as a walkie-talkie communication from an emergency scene becomes a signal that is amplified throughout the medical community on call, including the many specialties in the hospital that are available 24/7. This is what makes HCMC a Level 1 Trauma Center.
As soon as a call comes into the HCMC emergency department that a patient who requires this level of care is inbound, an overhead page goes out through the department intercom: “Stab. Room personnel to the Stab. Room, trauma, ten minutes; Stab. Room personnel to the Stab. Room, trauma, ten minutes.” Doctors, nurses, and healthcare assistants make their way over to the stabilization room, key their card in, and begin preparing. The doctors and nurses don special isolation scrubs and prepare instruments and devices for the incoming patient, and depending on how much or little is known about the injury or illness that has occurred, healthcare assistants may alert other specialties that are on-call 24/7 in the hospital. Specialties called on include trauma surgery, neurosurgery, orthopedic surgery, radiology, the stroke team, the pediatric team, the burn team, and even a team that uses a bariatric chamber to treat carbon monoxide poisoning. In this way, what most often begins as a walkie-talkie communication from an emergency scene becomes a signal that is amplified throughout the medical community on call, including the many specialties in the hospital that are available 24/7. This is what makes HCMC a Level 1 Trauma Center.
As emergency medicine doctors and nurses finalize their preparations for the incoming patient, they stand around the bedside, fully gloved and gowned, instruments and medications at the ready. All is quiet. Palpable anticipation, and after a few minutes dampened chatter, fill the air. Then, paramedics or flight medics burst through the double doors at the entrance to the stabilization room, wheeling in the patient quickly and confidently.
For ten to thirty seconds, every single person in the room gives their undivided attention to the paramedics as they efficiently provide a description of the patient’s situation and care provided in  the interim from the emergency scene to the hospital. It is my responsibility to create an accurate transcription of this pre-hospital care summary. Many specialty teams that are still en route to the stabilization room and other entering healthcare providers will look at the document I’m composing to understand the situation, and physicians will later use this as an aid to create a detailed chart of their interventions. Once the pre-hospital care is stated vocally, the patient is transferred from their stretcher onto a bed, and the team springs into action.
the interim from the emergency scene to the hospital. It is my responsibility to create an accurate transcription of this pre-hospital care summary. Many specialty teams that are still en route to the stabilization room and other entering healthcare providers will look at the document I’m composing to understand the situation, and physicians will later use this as an aid to create a detailed chart of their interventions. Once the pre-hospital care is stated vocally, the patient is transferred from their stretcher onto a bed, and the team springs into action.
On one level, there are standards of care and treatment algorithms in place that unequivocally determine what goes on and when in the stabilization room. Patterns of chief concerns and their accompanying medical interventions resonate throughout similar cases — the need to assertively manage the airway of a patient who has overdosed on opiates, the effort to deliver massive fluid resuscitation to a patient with major hemorrhaging, and the focus on protecting the neurological integrity of a patient with a potential traumatic brain injury. Yet despite basic consistencies in the management of trauma and severe illness, on a deeper level, each case is utterly extraordinary. There are twists and turns, unexpected assessment findings, and elaborate and sometimes inexplicable physiological responses from the patient that warrant consideration from many health professionals.
It is no exaggeration to say that many people in the room have spent the first half of their entire lives training to care for patients here. So for me, being without question the youngest, most inexperienced person on the team, getting to stand right at the foot of the bed is incredible. I see technical expertise interwoven with empathy in a way that is like simultaneously watching Einstein deriving general relativity, Van Gogh’s painting Starry Night, and Amelia Earhart flying through a thunderstorm. Here I feel that I have dual roles – first and foremost as a part of the medical team and with an immediate duty to provide any support within my scope of practice that will help the patient, and then as a student who, with the enormous privilege of getting to see the work that goes on in here, has an obligation on behalf of all of his future patients to learn all that he possibly can. Whenever it is appropriate, I ask questions. Whenever there’s room and I can do so without creating risk, I observe procedures. This constant observational learning and exposure to the thought processes involved in diagnosing and treating injury and disease is the most brilliant educational method I can imagine. Yet while this type of experience constitutes some of the most critical technical training I will ever obtain as an undergraduate, there are moments in the stabilization room that are far more valuable to me than understanding a physiological process or learning the nuances and pitfalls of a procedure. These are the moments of vulnerability and compassion that teach me, in the purest sense, what it means to be human.
Yet despite basic consistencies in the management of trauma and severe illness, on a deeper level, each case is utterly extraordinary.
 When someone in truly critical condition is brought to HCMC, when someone is on the brink of death, something peculiar happens. As physicians are rushing to simultaneously insert a breathing tube into their trachea, monitor their cardiac activity, and deliver chest compressions, as nurses and pharmacists line up with coolers of blood transfusions and medications in syringes and IV bags, and as residents and wide-eyed medical students observe and assist in procedures they will someday be leading, there’s a sense that we’ve arrived at the edge of something. We’ve arrived at a place where physiological mechanism merges with philosophical meaning, both in the face of a vast frontier that is present all around us. This frontier is the fundamental origin of our existence, it is what will happen to us when our magnificent yet finite bodies reach the end of their capacity, and it is utterly beyond our ability to comprehend. I think this unknown is the nature of life, and it is what makes our existence indescribably beautiful.
When someone in truly critical condition is brought to HCMC, when someone is on the brink of death, something peculiar happens. As physicians are rushing to simultaneously insert a breathing tube into their trachea, monitor their cardiac activity, and deliver chest compressions, as nurses and pharmacists line up with coolers of blood transfusions and medications in syringes and IV bags, and as residents and wide-eyed medical students observe and assist in procedures they will someday be leading, there’s a sense that we’ve arrived at the edge of something. We’ve arrived at a place where physiological mechanism merges with philosophical meaning, both in the face of a vast frontier that is present all around us. This frontier is the fundamental origin of our existence, it is what will happen to us when our magnificent yet finite bodies reach the end of their capacity, and it is utterly beyond our ability to comprehend. I think this unknown is the nature of life, and it is what makes our existence indescribably beautiful.
In the stabilization room, as we are working on our most critical patients, this unknown fills the room; it forms a focal point in the universe at which our incomplete, transient understanding of this world connects with whatever lies beyond, and it reaches out to our patients. I have played no prior role in these patients’ lives. I don’t understand what makes life meaningful to them, I cannot begin to appreciate the intricacies and qualities that define their character, and yet I find myself standing with them during one of the most personal, human moments of their existence. Having only just met them, I realize I am saying goodbye.
 After a patient passes, there is a quiet that settles throughout the room. Not a coordinated silence, but a few moments in which voices dissipate and the previously frantic atmosphere of the trauma bay calms down. Every single person in the room, at least once, casts their eyes on our friend, conveying a message of gratitude, humility, and reverence. Our patients may not have been surrounded by family members or friends, but when they pass, they are surrounded by people who appreciate the powerful moment of a fellow human entering the mysterious, terrifying, beautiful unknown. From this we are moved in a way that will remain with us for our entire lives.
After a patient passes, there is a quiet that settles throughout the room. Not a coordinated silence, but a few moments in which voices dissipate and the previously frantic atmosphere of the trauma bay calms down. Every single person in the room, at least once, casts their eyes on our friend, conveying a message of gratitude, humility, and reverence. Our patients may not have been surrounded by family members or friends, but when they pass, they are surrounded by people who appreciate the powerful moment of a fellow human entering the mysterious, terrifying, beautiful unknown. From this we are moved in a way that will remain with us for our entire lives.
When my shift draws to a close, I depart the stabilization room through its double doors, leaving team members, colleagues, and friends who have many hours to go in a place that never sleeps, and also leaving a piece of myself. As I bike back towards campus, my mind is filled with memories, emotions, and an understanding that truly the reason I do all that I do is for my patients, whose struggles, victories, and final moments I have the unimaginable privilege of participating.
Jack Hedberg is a stabilization room recorder at HCMC and a student at the University of Minnesota.
10 Comments
Leave a Comment
You must be logged in to post a comment.


Wonderful writing. Excellence descriptions of technical and compassionate care. I’ve been there many times with my husband.
Excellently written!
Beautifully written – our world will be lucky to have you as a physician someday!
Your writing is so touching, Jack!! Your compassion and care is what going to make you a great physician one day!!!
Thank you very much Ms. Warner! I’m glad you enjoyed it.
Thank you Ms. Schumacher!
Thank you very much Ms. Malaga; I’m glad you enjoyed it.
Great article. Wonderfully written! It’s the compassionate care that drives us to do what we do not the sexy procedure at the bedside. Never confuse the two things. It’s about the patients that come through those double doors and giving them compassionate care when they are the most vulnerable.
Absolutely amazing! Thank you for the wonderful portrayal of our department and care! I truly believe everyone at Hennepin brings their best to work everyday and it shows in our care! Thank you for this article!
Absolutely beautiful!!!