
Family Medicine
Three-Year ACGME-accredited Residency
Inpatient and ambulatory medicine serving a diverse, safety-net population
Gender-affirming care of adult and adolescent patients
Certification in integrative and holistic medicine
Training in high-risk OB, gestational diabetes, and prenatal and parenting group visits
Nationally recognized family-centered, culturally responsive integrative adolescent care
Training in osteopathic manipulative therapy for osteopathic and allopathic residents
Opportunities for rural and global health rotations
Family Medicine National Innovation in Continuity Clinic Experience pilot project participating program. In collaboration with the American Board of Family Medicine and the Association of Family Medicine Residency Directors.
Program Overview
Training family physicians for urban, rural, and global practice
Established in 1969 and graduating over 550 graduates to date, the Family Medicine Residency at Hennepin Healthcare remains at the forefront of primary care. Residents gain immediate, hands-on experience working with a diverse patient population. Our residents use the latest technology and learn from dedicated teaching staff and specialist colleagues. Our program features holistic and integrative medicine, full-spectrum women’s health, POCUS, sports medicine, geriatrics, and global health experiences.
Emphasis on Leadership
We emphasize resident leadership and a multidisciplinary approach to patient care that builds strong, collaborative relationships at all levels. Our graduates develop clinical expertise, effective communication, leadership skills, and practical management techniques. Upon graduation, they pursue a wide variety of paths, including fellowships and teaching faculty positions.
Opportunities
Family Medicine residents enjoy a weekly academic half-day of protected time to focus on workshops, procedures, and research. Resident wellness is a top priority. Our Wellness curriculum focuses on developing skills across multiple realms to prevent and combat burnout.
- Well-developed Health Care Home program launched and accredited in 2011 by the Minnesota Department of Health.
- Procedural training in OB-GYN procedures, skin biopsies, colposcopies, sports injury casting, POCUS, and more
- Full Spectrum reproductive health care including abortion care.
- Certification in Integrative Medicine using a curriculum developed by the University of Arizona Fellowship in Integrative Medicine.
- Sports medicine training
- Multifaceted Centering Pregnancy and Parenting model for group prenatal and well-baby care. Evidence-based care that lowers pre-term birth rates.
- Urban and rural rotations, with opportunities for global health rotations. Recent international sites include Senegal, Tanzania, the Philippines, and Thailand.
What is the "community" in Community Medicine?
At Hennepin Healthcare, FMR Community Medicine is not just a rotation, but a rich experience embedded in our rotations, didactic and longitudinal curriculum as well as the core mission of our hospital and affiliated clinics.
Our residents connect with the community we serve by participating in community outreach projects and developing an advocacy project with their classmates that spans the full 3 years.
Curriculum Highlights
Interdisciplinary Team-Based Care
Whittier Clinic, the primary clinic for Family Medicine residents, offers many services on-site:
- Acupuncture
- Addiction Medicine
- Aqui – Para- Ti (wrap-around adolescent care for at-risk Latinx youths) Whittier Clinic Aqui Para Ti / Here for You - Hennepin Healthcare
- Chiropractic Care
- Community Health Workers
- Diabetes Education
- Lactation Consultants
- Nutrition
- Occupational Therapy
- PharmD consultation
- Physical Therapy
- POCUS (point of care ultrasound)
- Psychologists
- Sleep Medicine
- Social Work
- Specialist consultation (General Surgery, Cardiology, OB/GYN, Podiatry)
- Sports Medicine
Wellness
Resident well-being and resilience have been the focus of our program for nearly 20 years. Since many factors influence our sense of well-being, our model explores wellness across various domains: physical, psychological, spiritual, occupational, environmental, financial, social, and intellectual wellness. The bi-monthly, 90-minute wellness seminars aim to 1) build skills to help residents rebalance and reduce the effects of stress in their lives, and 2) provide experiential opportunities to implement strategies for restoration (e.g., mindfulness, breathing techniques, yoga, tai chi, walking meditation, cooking/nutrition). We also offer annual retreats and host a “Family & Significant Other Orientation” at the beginning of the academic year.
Other resources offered within the greater Hennepin Healthcare Graduate Medical Education system include a Resident Integrated Service Environment (aka, RISE). RISE serves as a well-being resource hub with on-site providers specifically available for residents. The resources available to residents include primary care, psychiatry, psychology, and financial planning. These on-site resources help reduce the access barrier and address common concerns influencing well-being.
Simulation
All residents participate in our innovative curriculum that utilizes high and low-tech interactive learning modalities (from high-fidelity simulation and task trainers to case-based learning sessions) to teach procedural and clinical skills, and medical knowledge, and promote inter-professional collaboration. These sessions are interspersed throughout the 3 years of residency. This curriculum enhances team-based care, addresses systemic problems by producing possible system solutions, works to enhance patient safety, and ultimately improves patient care.
Additionally, our FM team participates in the multidisciplinary maternity care sims on Labor and Delivery.
Sports Medicine
Within our sports medicine curriculum, residents learn from faculty who are fellowship-trained in sports medicine. They rotate in the musculoskeletal clinics both within and outside of the Hennepin system. Additionally, during the PGY-2 year, residents participate in a didactic course at the University of Minnesota. Residents may also assist team physicians with local high school sports teams.
Behavioral Science
The Behavioral Science curriculum focuses on integrating a biopsychosocial framework into medical care in an effort to meet the individual needs of patients and families.
Longitudinal curriculum:
- Monthly seminars during core conference didactics
- Patient-Centered Grand Rounds
- Simulation training
- 1:1 observation
- Video Review
- Workshops (e.g., motivational interviewing)
- “Enhanced Care Clinic” (multidisciplinary case conference)
- Project ECHO (multidisciplinary case conference for addiction & chronic pain)
- Week-long training at Betty Ford Treatment Center
Block Rotation: Residents in their 2nd or 3rd year may choose elective rotations with Psychiatry Consult-Liaison Service and/or Addiction Medicine.
Clinic-based Learning: Residents have opportunities to consult with and provide team-based care alongside several disciplines: psychologists, consulting psychiatrists, addiction specialists, social workers, a team of community health workers, RN care manager, and financial counselors.
Group visits
Residents receive training in medical group visits throughout their training. All residents facilitate a Centering Pregnancy and Centering Parenting group, in which they care for a group of prenatal patients through their pregnancies, deliveries, and into the first year of well childcare.
Residents also work with our Integrative Faculty during their group visits which include “Aging Gracefully” and other lifestyle-related groups. They also have the opportunity to partner with these faculty to design and implement a group visit in an area of special interest during elective time.
Integrative Medicine
In addition to embedding principles of Integrative Medicine into our core curriculum, residents may participate in 200 hours of online training through the Andrew Weil Center for Integrative Medicine and complete certification in this discipline.
At the end of PGY-1, residents can opt for additional, focused training in Integrative Medicine outside the core curriculum, using several formats and modalities during their PGY-2 and PGY-3 years.
Clinic sessions:
- Performing integrative medicine interviews with patients;
- Populating functional timelines and matrix;
- Formulating patient-centered integrative health treatment programs; and
- Implementing integrative medicine longitudinally in their primary patients.
Personal study and self-care:
- Institute for Functional Medicine (IFM) core lectures and videos;
- Identifying a personal focus area to study, such as women’s health, herbal therapy, nutrition, or cardio-metabolic syndrome;
- Self-evaluation throughout the rotation on diet, digestion, exercise, energy, sleep, stress, support;
- Observing and experiencing the treatments of Complementary and Alternative Medicine (CAM) practitioners who work at Whittier Clinic, such as chiropractic, acupuncture, physical therapy, and traditional healers;
- Participating in the “Integrative Medicine 4 Us” and Pillsbury House for community service; and
- Delivering a journal club lecture on an integrative health topic.
Geriatrics
Our longitudinal geriatric curriculum prepares our graduates to provide the highest quality care for older patients - an important skill, as more than 20 million adults over age 85 are estimated to need medical care by 2050.
In addition to the traditional core curriculum and direct patient care, residents can opt for additional, focused training in Geriatrics towards the end of the PGY-1 year, using a longitudinal approach during their PGY-2 and PGY-3 years. These residents take on additional geriatric rotations and gain experience in nursing home administration, hospice, and palliative care, and the skills needed to provide care to ambulatory older patients.
Procedures
All residents rotate in the Whittier Clinic minor procedure clinic. Residents may perform joint injections, basic and advanced skin procedures, vasectomies, and other procedures in this clinic. Additionally, point-of-care ultrasound (POCUS) and contraceptive management procedures are integrated longitudinally into the curriculum. Procedural care is also part of training in the Simulation Center.
Elective Rotations including rural or global health experiences
We offer a wide variety of elective opportunities during all three years of residency. These encompass rotations both at Whittier Clinic as well as various sub-specialty clinics at Hennepin Healthcare. If you do not find what you are looking for, our residents are able to create their own electives, under faculty guidance, to design a learning experience specific to their interests. Additionally, we have ongoing relationships with international sites and will soon participate in an institution-wide Global Health Pathway. There is a rural elective site in Montevideo, Minnesota.
Didactic Opportunities
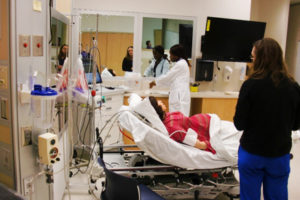 Family Medicine residents enjoy a weekly academic half day of protected time (five hours) to focus on didactics, procedures, and research.
Family Medicine residents enjoy a weekly academic half day of protected time (five hours) to focus on didactics, procedures, and research.
Our program features a strong emphasis on obstetrics, and the inclusion of integrative medicine, geriatric care, and home health care principles across the curriculum.
Wednesday Core Conference
- Protected half-day of didactic, academic learning organized around organ systems
Special Workshops and Focused Learning Opportunities
- Interdisciplinary Simulation and Education Center Learning (SIM)
- Hands-on, situational learning to build teamwork and skills
- Takes place in Hennepin Healthcare’s state-of-the-art Interdisciplinary Simulation and Education Center
- Staged Diabetes Management
- Full day workshop to learn progressive management of diabetes patients
- Gestational Diabetes Management
- A half-day workshop to learn the management of patients with gestational diabetes
- Neonatal Resuscitation Program (NRP)
- Advanced Cardiac Life Support (ACLS)
- Advanced Life Support in Obstetrics (ALSO)
- Adolescent Workshop
- Intensive training for PGY-2 residents
- Specially trained high school students (generally those who are peer educators) role play teens visiting the doctor
- Residents interview and interact with the teens, and then gain real-time feedback from both the teens and faculty facilitators
- Integrative Medicine/Functional Medicine
- 200-hour self-learning course offered by University of Arizona Fellowship in Integrative Medicine
- Hands-on clinical experiences with fellowship trained Integrative Medicine faculty, including group visits
- CME days available
About Our Faculty
Experienced and Diverse Faculty Focused on Teaching
Twenty-three teaching faculty lead the Family Medicine residency, including geriatrics, integrative medicine, sports medicine, and international health. Many are nationally recognized leaders in their fields with extensive clinical and academic healthcare experience. More than 70% of our teaching faculty completed Faculty Development Fellowships at the University of Minnesota, and all hold university appointments.
Program Leadership
- Kimberly Petersen, MD, Interim Residency Program Director, Director of Family Medicine Inpatient Services, Hennepin Healthcare
- Analisa Calderon, MD, Associate Program Director, Hennepin Healthcare
- Sadhana Vanka, MBBS, Associate Program Director, Sleep Medicine, Hennepin Healthcare
Program Faculty
- Allyson Brotherson, MD, Chair of Family Medicine Department
- Andres Camacho, MD
- Chandra Cherukuri, MBBS, Vice Chair of Family Medicine Department, Geriatrics, Sleep Medicine
- Jason Como, MD
- David Councilman, MD
- Susan Haddow, MD, ABIHM, Integrative Medicine
- Susan Hasti, MD
- Marchion Hinton, PhD, Assoc Vice Chair, Behavioral Science
- Michelle Karsten, MD
- Kirsten Morissette, MD
- Ayham Moty, MD
- Nancy Newman, MD, Behavioral Science
- Tsewang Ngodup, MD, Geriatrics
- Kara Parker, MD, Integrative Medicine
- Lourdes Pira, MD
- Rachel Rapacz, MD
- Kristin Schwacha, DO
- Veronica Svetaz, MD, MPH, Adolescent Medicine
- Praveen Tupakula, MBBS, Informatics, Sr Medical Director, HHS Primary Care Ring
- Jenna Walters, MD
Community Preceptors
- Luis Barillas Schwank, MD
- Gisele Bouroncle, MD
- Thomas Bracken, MD
- Natalie Hayes, MD
- Didi Koka, MD
- Bernice Lee, MD
- Ken Joslyn, MD
- Gillian Mojica-Martinez, MD
- Jerrod Nordberg, MD
- Michelle Schabert, MD
Rotations
View the Rotation Schedule (PDF)
PGY-1
The first year of the Family Medicine Residency program prepares residents for inpatient medical and emergency care, including obstetrics and pediatrics, and sets the groundwork for essential outpatient skills and practice. Our residents work collaboratively with other Hennepin Healthcare residency programs, building relationships and taking advantage of broad educational opportunities within our healthcare system. Family Medicine residents also teach medical students on the inpatient service.
The inpatient Family Medicine Services includes adult, pediatric, and obstetric patients from our own practice at Whittier Clinic, as well as patients from three additional Hennepin Healthcare primary care community clinics.
At Whittier clinic, G1 residents develop skills in outpatient primary care as they build their own practice panel. We use the “Clinic First” model which prioritizes continuity in the clinic by maintaining a stable clinic day that patients and residents can rely on.
Orientation occurs weekly during the first two months of training. During this time, residents participate in team-building and skill-building activities and learn essential skills for integration into the residency program.
PGY-2
PGY-2 residents take on a leadership role in the inpatient Family Medicine Service, monitoring the work of interns, and medical students and supervising the care of all inpatients under the guidance of faculty. A separate 4-week ultrasound rotation incorporates the use of point-of-care ultrasound in both the inpatient and outpatient settings.
Outpatient experiences are set at Whittier Clinic, as well as at Hennepin Healthcare’s specialty clinics, and include dermatologic, orthopedic, and gynecologic procedures as part of everyday practice. Ambulatory experiences include work at the Whittier procedure clinic, where residents learn procedures common to family medicine.
During PGY-2, residents begin a longitudinal experience at a local skilled nursing facility, developing continuity relationships with geriatric patients. Residents will also begin their Centering Pregnancy groups in the second year.
PGY-3
Our third year focuses intensively on continuity clinic practice at the Whittier Clinic location. Residents build their knowledge and apply their skills to care and management of patients with complex healthcare needs.
Outpatient rotations take advantage of Hennepin Healthcare’s various specialty clinics to address common primary care problems, such as rheumatology, geriatrics, ENT, cardiology, gynecology and urogynecology, outpatient pediatrics, and adolescent medicine.
Specific third-year experiences include:
- Outpatient pediatrics, working with community pediatricians;
- Outpatient procedures, including colposcopy, orthopedic, and gynecologic procedures;
- Specialty clinics in geriatrics, palliative care, and long-term care;
- Specialty clinics in urology, otolaryngology, and ophthalmology;
- Longitudinal care of nursing home patients and home visit care.
Residents maintain their inpatient skills with two months as the senior resident on the Family Medicine Service, with additional responsibilities for teaching and supervision of PGY-1 residents and medical students.
About Our Rotations
Diverse Rotations with Multiple Elective Options
Family Medicine Inpatient Service
One of the gems of our program, our team of Family Medicine residents and faculty run an independent, inpatient service drawing patients from 4 Hennepin Healthcare community clinics. We care for pediatrics, adult medicine, obstetrics, and newborns and actively manage all inpatient care plans, consults, and discharge planning. Although our residents take primary responsibility for patient management, we have in-house faculty 24 hours a day for back-up and teaching. Outside of the Family Medicine Service, all residents rotate in the ICU where they have the opportunity to work with faculty and residents from multiple other specialties.
Obstetrics
Family Medicine residents gain valuable experience with low- and high-risk pregnancies during their rotations. Residents rotate through one block under the guidance of the OB department during the first year. Opportunities for managing obstetrics occur on all FMS blocks (total of 7) and during night calls. Residents have opportunities to perform all OB procedures and manage laboring patients with a variety of high-risk needs.
All Family Medicine inpatient faculty practice obstetrics and several serve on multi-disciplinary committees to help foster better communication and patient care. Five faculty members are Advanced Life Support in Obstetrics (ALSO) instructors, including one nationally recognized ALSO Advisory Faculty.
Each resident takes the ALSO course in PGY-1 and again in PGY-2 or PGY-3 to enhance their skill and improve confidence when handling labor and delivery emergencies. Our residents have successfully managed dystocia and postpartum hemorrhage, and routinely cite the ALSO course as increasing their ability to manage these situations.
Another highlight is training in Centering Pregnancy. All residents co-facilitate their own prenatal group to learn this care model that has proven effective in lowering pre-term birth rates.
Pediatrics
Our training includes a wide variety of experiences in Pediatric care. Including 2 inpatient rotations at Hennepin Healthcare one at Minneapolis Children’s Hospital, and a dedicated rotation in the Pediatric ED. We offer a specific outpatient rotation with focused learning in both general and adolescent Pediatrics, Centering Parenting group visits as well as a robust pediatric population in the Whittier clinic.

Application Requirements
- Documents submitted through ERAS and the NRMP
- USMLE or COMLEX transcript
Selection Criteria
- Meet eligibility criteria for licensure in Minnesota. This requires passage of all components of the USMLE (or COMLEX) within three attempts.
- Meet the following USMLE or COMLEX exam requirements:
- Preference for a first-time pass on the USMLE steps 1 and 2
- Preference for a minimum score of 215
- International medical graduates must submit passing Step 1 and Step 2 scores before their applications will be considered.
- USMLE Step 2 or COMLEX Level 2 exam results are not required for current medical students but are preferred for interview selection. Please submit scores as soon as they are available. Passing scores must be submitted for ranking.
- Medical school graduation within 2 years of residency start date and medical school matriculation within 7 years of residency start date
- Medical schools must appear in one of the following directories:
- Letters of Recommendation (minimum 3) including at least one from a US clinical supervisor and preference for at least one from a Family Physician
- ECFMG certification for international medical graduates
- Citizenship, permanent residency, or ability to obtain a J-1 visa.
- Excellent written and spoken English language communication skills
- Qualified to begin work around June 10th of residency start year.
- Couples match applicants considered
Interview Information
- We will have an online (virtual) interview process for the Fall of 2023 Interview season. In-person Open Houses (Second Look Opportunities) will be available after the conclusion of interviews. During interviews, there will be an opportunity to meet program leadership, faculty, and residents, as well as a virtual tour of our community, hospital, and Whittier clinic.
- Our program will be participating in ERAS Program Signaling.
- Eligible applicants will be contacted to schedule interviews starting after the ERAS open date on a rolling basis as applications are reviewed. Due to the high level of interest in our program, we are not able to interview all applicants.
- Interview days are Tuesdays, Thursdays, and Fridays
- Interviews are required for admission to our program.
The Family Medicine Residency at Hennepin Healthcare is ACGME accredited.
What Sets Us Apart?
Diverse patient experience.
Residents treat a diverse cross-cultural population with a wide variety of chronic illnesses and acute issues. This ranges from diabetes, heart failure and heart disease to sports injuries to tropical infections.
Community and advocacy.
All residents will have the opportunity to participate in a community advocacy project as well as community events.
Strong inpatient and outpatient training.
Residents develop essential skills to manage hospitalized patients and help them transition to outpatient care. They also manage their own outpatient patient panel, as well as design and implement clinical quality improvement projects.
Holistic approach.
Our integrative medicine curriculum focuses treatment on the whole patient and demonstrates how to incorporate holistic concepts into regular practice. Outpatient training includes collaboration with care providers in acupuncture, physical therapy, behavioral health, and chiropractic care.
Advanced technology.
Hennepin Healthcare operates with Epic and has integrated electronic health records available in all locations. Our clinics feature up-to-date lab and radiology services, with access to additional services on the main HCMC campus. Residents train for real-life scenarios in our state-of-the-art simulation and education center, and we have an integrated point-of-care ultrasound (POCUS) curriculum.
Collegial, multidisciplinary environment.
Our residents work and learn within our family medicine department as well as in inter-departmental collaborative practices with the Internal Medicine, Emergency Medicine, Pediatrics, Surgery, and Ob/Gyn Departments. As an academic system, teaching, medical education, and research are priorities for faculty across our system.
About Our Facility
Whittier Clinic serves as the main site for family medicine residents. Whittier Clinic provides immediate, on-site access to everything from x-ray, ultrasound, and laboratory services to a dedicated support staff of social workers, physical therapists, interpreters, and other professionals.




